Introduction
This review is somewhat multi-disciplinary in nature. As you wrap up your reviews, one of the things I found useful was to create tons of different lists. Regardless of which test you're studying for, there are many questions that are organized differently than how one might go about learning a particular disease. As such, I started making lists of different ways to group otherwise disparate diseases that might show up as a test question, or at least help me remember a specific feature of the disease.
Because glaucoma is a potentially sight-threatening/blinding disease, it is important to know if a particular condition is associated with glaucoma in any way, so that appropriate screening can be initiated. While the following list is by no means comprehensive, it is a list that I started putting together while I was studying for the OKAP.
Another caveat is that each individual condition will likely be featured as many individual articles in the future. For the sake of brevity (which I have a hard time doing), I am purposefully not including significant details about each disease. I am still going to try to include images of each condition, since repetition and visual pattern recognition are vital to review, and I will try to include details about the pathophysiology of glaucoma and some basic information about each condition. Hopefully this list can serve as yet another scaffold for you to remember the copious amounts of information needed for testing and clinical practice.
For those who want to skip the pictures, I made a little summary table at the bottom of the article. Hope it helps!
Conditions Associated With Glaucoma
Oculodermal Melanocytosis (Nevus of Ota) (10%)
Image credit: Indian Journal of Dermatology, Venereology and Leprology.
- Nevus of Ota, or dermal melanocytosis, is a diffuse congenital blue nevus in the V1 and V2 dermatomes.
- It is typically unilateral (95%), and the risk of glaucoma is typically present on the same side as the nevus. The risk is fairly low (10%).
- Another concerning risk is the increased risk of uveal melanoma in patients with ocular involvement (1 in 400, especially in white patients).
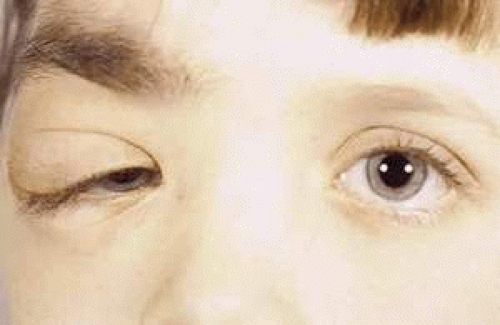
Sturge-Weber Syndrome (50-70%)
Image credit: MRCOphth.com
- Sturge-Weber Syndrome, or encephalofacial/encephalotrigeminal angiomatosis, is a sporadically-inherited phakomatosis that consists of facial cutaneous angiomas and ipsilateral leptomeningeal vascular malformations.
- The characteristic skin lesion, the port wine stain (nevus flammeus), consists of dilated and excessively numerous but well-formed capillaries in the dermis. It may be treated with pulsed dye laser.
- Glaucoma occurs in 50-70% of cases. The glaucoma is typically ipsilateral to the lesion.
- The mechanism for glaucoma is a combination of increased episcleral venous pressure, hyperemia of the ciliary body causing increased aqueous production, and anomalous angle anatomy.
- Management of the glaucoma is challenging, as there is an increased risk of expulsive choroidal hemorrhage during surgery.
Plexiform Neurofibroma (50%)
Image credit: Cannon TC, Carter KD, Brown HH. Neurogenic tumors of the orbit. Ento Key.
- Plexiform neurofibromas of the eyelid are often seen as part of the phakomatosis, neurofibromatosis type 1 (von Recklinghausen disease).
- They are highly specific to neurofibromatosis type 1 but are only present in about 30% of cases.
- If they are large enough, they can induce against-the-rule astigmatism (flattening superiorly), and even amblyopia (deprivational or refractive).
- Patients with plexiform neurofibromas of the eyelid may have glaucoma in the ipsilateral eye (seen in 50% of patients). Congenital iris ectropion is also implicated in ipsilateral glaucoma.
- The pathophysiology of glaucoma in neurofibromatosis type 1 is associated with abnormal trabecular meshwork development and synechial angle closure.
I hope to have some more detailed reviews of the phakomatoses soon, which should hopefully put some of these features together better.
Microcornea (20%)
Image credit: University of Iowa, EyeRounds.org.
- Microcornea is defined as a corneal diameter < 10 mm in an adult (< 9 mm in children).
- The pathogenesis of microcornea is unclear. Hypothesized mechanisms include fetal arrested development or optic cup overgrowth.
- Glaucoma is a common complication of microcornea. The primary mechanism of glaucoma in patients with microcornea is angle closure due to the narrowed and crowded angle. However, 20% of patients with microcornea that do not have angle closure will develop open-angle glaucoma. The mechanism for open angle glaucoma is not listed in the texts that I have (if someone has a reference to add, e-mail me!).
Sclerocornea (50%)
Image credit: Pinterest
- Sclerocornea is the scleralization of the cornea.
- It is typically bilateral (90%).
- Glaucoma occurs in 50% of cases, and is a result of abnormal angle anatomy.
Peters Anomaly (50%)
Image credit: studyblue.com.
- Peters anomaly refers to the congenital absence of the corneal endothelium and Descemet's membrane.
- It occurs both as a developmental anomaly from external toxic influences (such as fetal alcohol syndrome) and genetic abnormalities, which can be inherited or occur sporadically.
- Glaucoma is a frequent sequelae, which is typically related to abnormal angle development or narrowed angle (as microcornea may occur).
Posterior Polymorphous Corneal Dystrophy (40%)
Posterior polymorphous corneal dystrophy, with vesicular-type lesions noted.
Image credit: University of Iowa, EyeRounds.org.
- Posterior polymorphous corneal dystrophy (PPMD or PPCD) is an autosomal dominant-inherited corneal dystrophy associated with abnormal development of corneal endothelium.
- The corneal endothelium may have epithelial-like features, such as microvilli, keratin, desmosomes, and may proliferate, leading to multiple layers of cells seen on histopathology (which differs from the single layer of normal endothelium).
- While the mechanism and actual histopathology differs from iridocorneal endothelial (ICE) syndrome, it does share some similar features, such as angle-closure glaucoma and open angle glaucoma.
Axenfeld-Rieger Syndrome (50%)
Axenfeld-Rieger syndrome. Note the anteriorly displaced Schwalbe line (posterior embryotoxon), thinned and stretched iris that leads to corectopia, and peripheral anterior synechiae in the angle that may cause glaucoma.
Image credit: molvis.org.
- Axenfeld-Rieger syndrome is a collection of anterior segment anomalies (anterior segment dysgenesis) that consists of bilateral congenital abnormal development of the angle, iris, and trabecular meshwork. In severe cases, facial and systemic developmental anomalies are also seen (Rieger syndrome).
- Glaucoma occurs in 50% of cases, and occurs as a result of a combination of anterior segment dysgenesis and peripheral anterior synechiae that causes angle closure.
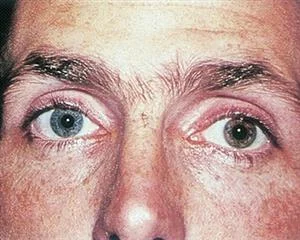
Fuchs Heterochromic Iridocyclitis (15%)
Iris heterochromia.
Image credit: American Academy of Ophthalmology.
- Fuchs heterochromic iridocyclitis is an idiopathic unilateral chronic-recurrent iridocyclitis.
- Glaucoma is a common sequelae of Fuchs heterochromic iridocyclitis; the pathophysiology of the glaucoma is unknown.
Juvenile Xanthogranuloma (80%)
- Juvenile xanthogranuloma is a systemic xanthogranulomatous condition (inflammation against lipids) that may result in iris heterochromia, spontaneous hyphemas, and skin lesions.
- Although glaucoma is extremely common (in 80% of cases), the pathophysiology is unknown.
Image Links
- Parmley VC, George DP, Fannin LA. Juvenile xanthogranuloma of the iris in an adult. Arch Ophthalmol. 1998;116(3):377-379. doi:10.101/archopht.116.3.377.
- Flockerz E, Hager T, Seitz B. Intraocular juvenile xanthogranuloma of the iris in an adult patient. American Journal of Ophthalmology Case Reports. 2017;5:73-75. doi:10.1016/j.ajoc.2016.12.003.
Aniridia (50%)
Image credit: University of Iowa, EyeRounds.org.
- Aniridia is a developmental anomaly that is often associated with other ocular developmental problems and may have genetic or environmental causes.
- Glaucoma is common. The pathophysiology of glaucoma in aniridia is angle-closure from trabecular meshwork occlusion by hypoplastic iris stump.
Summary
Here is a quick-reference chart for these conditions:
References and Additional Resources
- Basic and Clinical Science Course, Section 6: Pediatric Ophthalmology and Strabismus. American Academy of Ophthalmology, 2015.
- Basic and Clinical Science Course, Section 7: Orbits, Eyelids, and Lacrimal System. American Academy of Ophthalmology, 2015.
- Basic and Clinical Science Course, Section 8: External Disease and Cornea. American Academy of Ophthalmology, 2015.
- Basic and Clinical Science Course, Section 9: Intraocular Inflammation and Uveitis. American Academy of Ophthalmology, 2015.
- Basic and Clinical Science Course, Section 10: Glaucoma. American Academy of Ophthalmology, 2015.
- Hale C. Nevus of Ota. PathologyOutlines.com, 2017.
Did we miss any conditions that may be associated with glaucoma? Are there other tips that may be helpful for remembering these conditions? Leave a message or contact us!