Follicular conjunctivitis is one of those topics that always seems to pop up on exams. Because questions can be asked about the pathology and differential diagnosis, this is a topic that probably should be very familiar to you.
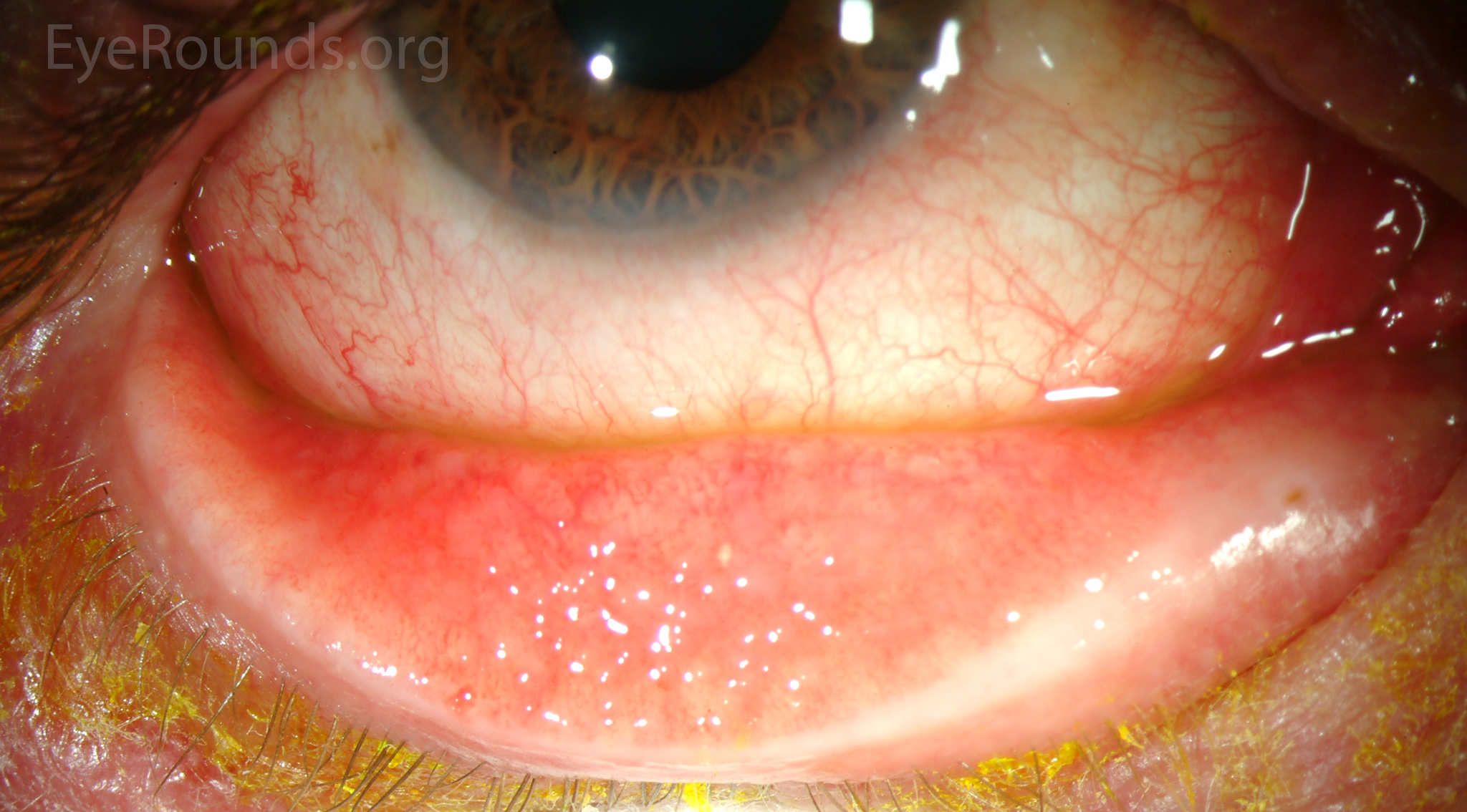
Follicular conjunctivitis.
Image credit: University of Iowa, EyeRounds.org.
Histopathology
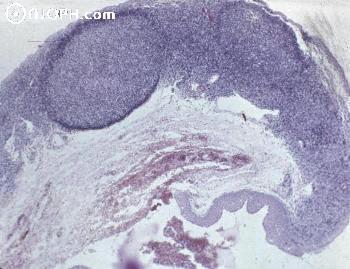
Histopathology of follicular conjunctivitis.
Image credit: Online Journal of Ophthalmology.
There probably isn't a ton to say about the histopathology of follicular conjunctivitis, other than that you may need to be able to recognize what it looks like. The typical histopathologic description is lymphoid follicles in the conjunctiva, which have 3 components:
- Corona: the outer layer, composed of darker blue, mature lymphocytes and plasma cells.
- Stroma: the middle layer, composed of lymphocytes and plasma cells.
- Germinal center: the inner layer, which is typically pale, and full of immature lymphocytes.
Differential Diagnosis
For some reason, the different causes of follicular conjunctivitis are very testable - probably because we see follicular conjunctivitis fairly often, and we need to have a somewhat broad differential diagnosis when we see this in our clinics.
For example, I had a patient who presented with follicular conjunctivitis (all identifying details changed to maintain HIPAA compliance). They had a history of "pink eye" for over 1 month, which had previously been treated with topical drops of various kinds. I had to make sure the patient wasn't using a drop that might cause the follicular conjunctivitis, but also start probing for other potential etiologies (recent infections, sexual history, travel to countries endemic to trachoma, poultry handling, etc.).
The differential diagnosis includes the following:
- Adenovirus: remember that subtypes D, 8, 19, and 37 cause epidemic keratoconjunctivitis
- Acute hemorrhagic conjunctivitis: there are 4 agents that can cause AHC, listed below
- Enterovirus 70 (which can cause a polio-like syndrome)
- Coxsackievirus A24
- Adenovirus subtype 11
- Adenovirus subtype 21
- Chlamydia
- Drugs
- Dipivefrin
- Neomycin
- Idoxuridine
- Trifluridine
- Atropine
- Sulfa-derivative antibiotics
- Brimonidine
- Herpesvirus
- Lyme (stage 1)
- Molluscum contagiosum (most common cause of unilateral follicular conjunctivitis)
- Measles
- Mumps
- Moraxella: one of the major causes of angular blepharitis
- Newcastle's Disease: this is a disease of poultry handlers
It's a pretty long list, and while I learned this list via a mnemonic, I unfortunately don't have permission to share it. I've highlighted the agents that I think are most important to consider when evaluating follicular conjunctivitis.
Treatment
Treatment of follicular conjunctivitis is largely determined by the cause (Azithromycin/doxycycline/erythromycin for chlamydia, excision of molluscum lesion, d/c offending agent, etc.). The conjunctivitis may take weeks to resolve.
References and Additional Reading
- Basic and Clinical Science Course, Section 4: Ophthalmic Pathology and Intraocular Tumors. San Francisco: American Academy of Ophthalmology, 2015.
- Basic and Clinical Science Course, Section 8: External Disease and Cornea. San Francisco: American Academy of Ophthalmology, 2015.
- Ehlers JP, Shah CP, eds. The Wills Eye Manual: Office and Emergency Room Diagnosis and Treatment of Eye Disease, 5th Edition. Philadelphia: Lippincott Williams & Wilkins, 2008.
Am I missing anything about follicular conjunctivitis that should be mentioned? Do you have any other tips or hints, or suggestions for new topics? Leave a comment or contact us!