Funny-looking optic discs are a "fun" diversion in an ophthalmology clinic (sarcasm implied here). What was initially a routine exam immediately turns into an agonizing "is this normal or not" exercise. Part of the angst that comes from seeing anomalous optic discs is that some of the congenital disc anomalies are associated with systemic diseases. If there is concurrent visual field loss or decreased visual acuity, the challenge becomes deciding if those defects in the visual system are due to the anomalous nerve, or if there is some other ophthalmic cause that we don't want to miss.
Because there are a few associated systemic conditions that we need to know as part of our training, there is certainly some possibility that a question or two may address these congenital disc anomalies. Fortunately, although there are many more than will be listed in this article, there are essentially 6 congenital disc anomalies that you should be familiar with before you take the OKAP.
As always, my disclaimer is that there is no guarantee that this topic or anything associated it will actually be on the OKAP. The topics I'm choosing to discuss come straight from the OKAP content outline provided by the AAO, so hopefully it's not just me who thinks these topics are important.
This ended up being a somewhat detailed summary that probably has more information that you absolutely need. For those people wishing to just get the short summary, just skip to the bottom of the article for a table.
Optic Nerve Hypoplasia
Optic nerve hypoplasia.
Image credit: University of Iowa, EyeRounds.org, hosted at the University of Arizona.
Key Facts
- Optic nerve hypoplasia is the most common optic disc anomaly encountered in ophthalmic practice.
- It is bilateral in 75% of cases.
- Mothers of people with optic nerve hypoplasia may have certain risk factors:
- Diabetes
- Alcohol abuse (fetal alcohol syndrome)
- Illicit drug abuse
- Medication use: quinine, anticonvulsants
- Certain infections: CMV, hepatitis B
Clinical Presentation
- Visual acuity is highly variable; there are many people with ON hypoplasia and normal vision, just as there are people with ON hypoplasia and profoundly poor vision.
- The visual field pattern is typically generalized constriction with localized defects.
Systemic Associations
A patient with optic nerve hypoplasia and absent septum pellucidum. An absent septum pellucidum is not indicative of any specific pathology.
Image credit: Al-Senawi R, Al-Jabri B, Al-Zuhaibi S, Al-Azri F, Al-Yarubi S, Harikrishna B, Al-Futaisi A, Ganesh A. Septo-optic dysplasia complex: Clinical and radiological manifestations in Omani children. Oman J Ophthalmol [serial online] 2013 [cited 2016 Feb 15];6:193-8. Available from: http://www.ojoonline.org/text.asp?2013/6/3/193/122277.
Posterior pituitary ectopia (arrow head). Note the relative hypointensity of the pituitary gland, and the hyperintensity of the posterior pituitary stalk.
Image credit: Al-Senawi R, Al-Jabri B, Al-Zuhaibi S, Al-Azri F, Al-Yarubi S, Harikrishna B, Al-Futaisi A, Ganesh A. Septo-optic dysplasia complex: Clinical and radiological manifestations in Omani children. Oman J Ophthalmol [serial online] 2013 [cited 2016 Feb 14];6:193-8. Available from: http://www.ojoonline.org/text.asp?2013/6/3/193/122277.
- Pituitary endocrine abnormalities (growth hormone deficiencies are the most common), are present in over 60% of cases.
- Over 45% of people with optic nerve hypoplasia have abnormalities on their MRI (cerebral or pituitary abnormalities)! An MRI is indicated in all patients who are found to have optic nerve hypoplasia.
- Caveat: an argument could be made that asymptomatic adult patients who are found to have ON hypoplasia can be observed expectantly, since any pituitary abnormalities would have manifested in childhood. However, for the sake of the test, an MRI of the brain or endocrine evaluation is the answer choice if they show a picture of ON hypoplasia and ask what test to order.
- Posterior pituitary ectopia is seen in 15% of cases. This is described as hypointensity of the pituitary gland and posterior hyperintensity. It is almost pathognomonic of anterior pituitary deficiency with normal posterior pituitary function.
- No signal from the posterior pituitary is predictive of diabetes insipidus.
- Transphenoidal basal encephalocele may be seen on MRI.
- Suprasellar tumors may also been seen.
Select Associations
- PAX6 mutations - aniridia may be another clinical finding.
- Fetal alcohol syndrome
- Astigmatism
- Duane syndrome
- Klippel-Trenaunay-Weber syndrome
- Goldenhar syndrome
- Aicardi syndrome
Histopathology
Histopathology of optic nerve hypoplasia. It is described as decreased number of ON axons with normal mesodermal elements and glial supporting tissue.
Image credit: pathguy.com.
- Histopathologically, optic nerve hypoplasia has a decreased number of optic nerve axons with normal mesodermal elements and glial supporting tissue.
Septo-Optic Dysplasia (De Morsier Syndrome)
- Consists of the triad: ON hypoplasia, absent septum pellucidum/agenesis of corpus callosum, and pituitary dwarfism
Topless Disc Syndrome (Superior Segmental Optic Nerve Hypoplasia)
Superior segmental optic nerve hypoplasia.
Image credit: University of Iowa, EyeRounds.org.
Inferior visual field defects associated with superior segmental optic nerve hypoplasia.
Image credit: Fovea.ir.
- "Topless disc syndrome" refers to isolated superior segmental optic nerve hypoplasia, which is often associated with an inferior visual field defect.
- It is associated with diabetic mothers.
Tilted Discs
Tilted Disc.
Image credit: StudyBlue.com.
Goldmann perimetry demonstrating the pseudo-bitemporal hemianopic defect, preferentially affecting the mid-sized isopters, not respecting the vertical midline (arrows).
Image credit: Manfre L, Vero S, Focarelli-Barone C, Lagalla R. Bitemporal Pseudohemianopia Related to the ‘‘Tilted Disk’’ Syndrome: CT, MR, and Fundoscopic Findings. AJNR Am J Neuroradiol 1999;20:1750-1751.
- Tilted discs are fairly common, especially in cases of high myopia.
- They are usually bilateral (80%).
- The superotemporal aspect of the optic nerve is typically elevated, which can mimic optic nerve edema.
- There can be situs inversus of the retinal vessels (increased branching of the retinal vessels nasally).
- Myopic astigmatism can be present, which is caused by a combination of irregular corneal curvature (K's) and posterior staphylomas.
- Bitemporal visual field defects may be present on automated perimetry, which typically do not respect the vertical midline and may preferentially involve the superotemporal visual fields. On Goldmann perimetry, only the mid-sized isopters are affected.
- On histopathology, there is oblique insertion of the optic nerve, elevation of superotemporal disc, and posterior ectasia inferiorly.
- Tilted nerves are independently associated with suprasellar tumors, and craniosynostoses (specifically Crouzon and Apert syndromes).
Optic Pit
Optic pit. Note the inferotemporal location of the pit.
Image credit: mrcophth.com.
Large macular serous retinal detachment in association with an optic pit.
Image credit: University of Iowa, EyeRounds.org.
- Optic pits may be inherited in an autosomal dominant fashion.
- They are typically unilateral (85%).
- The most common visual field defect seen is a paracentral arcuate scotoma connected to an enlarged blind spot.
- The histopathologic description of an optic nerve pit is herniation of dysplastic retina into a collagen pocket with a defect in the lamina cribrosa.
- Serous retinal detachment is a sight-threatening complication (up 50% in some case series). The source of the fluid is controversial and has been proposed as originating either from CSF or from the vitreous.4 Treatment is challenging, as laser photocoagulation alone is not always effective, and patients may require a pars plana vitrectomy with or without gas tamponade with laser photocoagulation.
SD-OCT showing a large serous retinal detachment in the case of a optic pit.
Image credit: University of Iowa, EyeRounds.org.
Optic Nerve Coloboma
Optic nerve coloboma.
Image credit: Online Journal of Ophthalmology.
- Optic nerve colobomas are the most common segmental form of optic nerve hypoplasia encountered clinically.
- It occurs as a result of incomplete closure of the embryonic fissure (which begins to close at day 33 of gestation). As such, optic nerve colobomas occur inferiorly, and may be associated with colobomas of the retina, choroid, and even anterior structures such as the lens or iris.
- Optic nerve colobomas are associated with defects in the PAX6 gene.
- It is associated with microphthalmos and serous retinal detachments. Retinal/choroidal colobomas are associated with rhegmatogenous retinal detachments.
- It is described histologically as intrascleral smooth muscle strands oriented concentrically around the distal optic nerve, with heterotopic adipose tissue within and adjacent to the optic disc.
- Systemically, optic nerve colobomas are associated with CHARGE, Aicardi syndrome, Goldenhar syndrome, and linear sebaceous nevus syndrome.
Morning Glory Disc Anomaly
Morning glory disc anomaly.
Image credit: Research Gate.
Morning glory flower.
Image credit: www.formlainc.com.
The Morning Glory pool at Yellowstone.
Image credit: Wikipedia.
- The morning glory disc anomaly named because it closely resembles the morning glory flower. There is also a geyser in Yellowstone called Morning Glory for the same reason.
- The characteristic feature of the morning glory disc anomaly is the abnormally straight retinal vessels that emanate from the disc margin (rather than from a central vessel).
- They are typically unilateral, present more frequently in females, and are associated with poor vision (20/200-count fingers).
- A white glial "tuft" may be seen, which may help to distinguish this from one of the other optic nerve anomalies.
- Serous retinal detachments are associated with this anomaly (30%), and there can also be subretinal neovascularization within the area of pigmentary disturbance surrounding the disc.
Systemic Associations
- Transsphenoidal basal encephaloceles are strongly associated with the morning glory disc anomaly. These encephaloceles are associated with endocrine dysfunction related to hypopituitarism.
- Moyamoya syndrome and ipsilateral intracranial vascular dysgenesis (specifically hypoplasia of the carotid and major cerebral arteries) may be seen.
- Morning glory anomaly has also been associated with the PHACE syndrome, which should be considered if there is an ipsilateral facial hemangioma (females only).
Workup
- All patients found to have a morning glory optic nerve anomaly should undergo neuroimaging with an MRI and MRA of the brain (with and without contrast) as well as an endocrine evaluation.
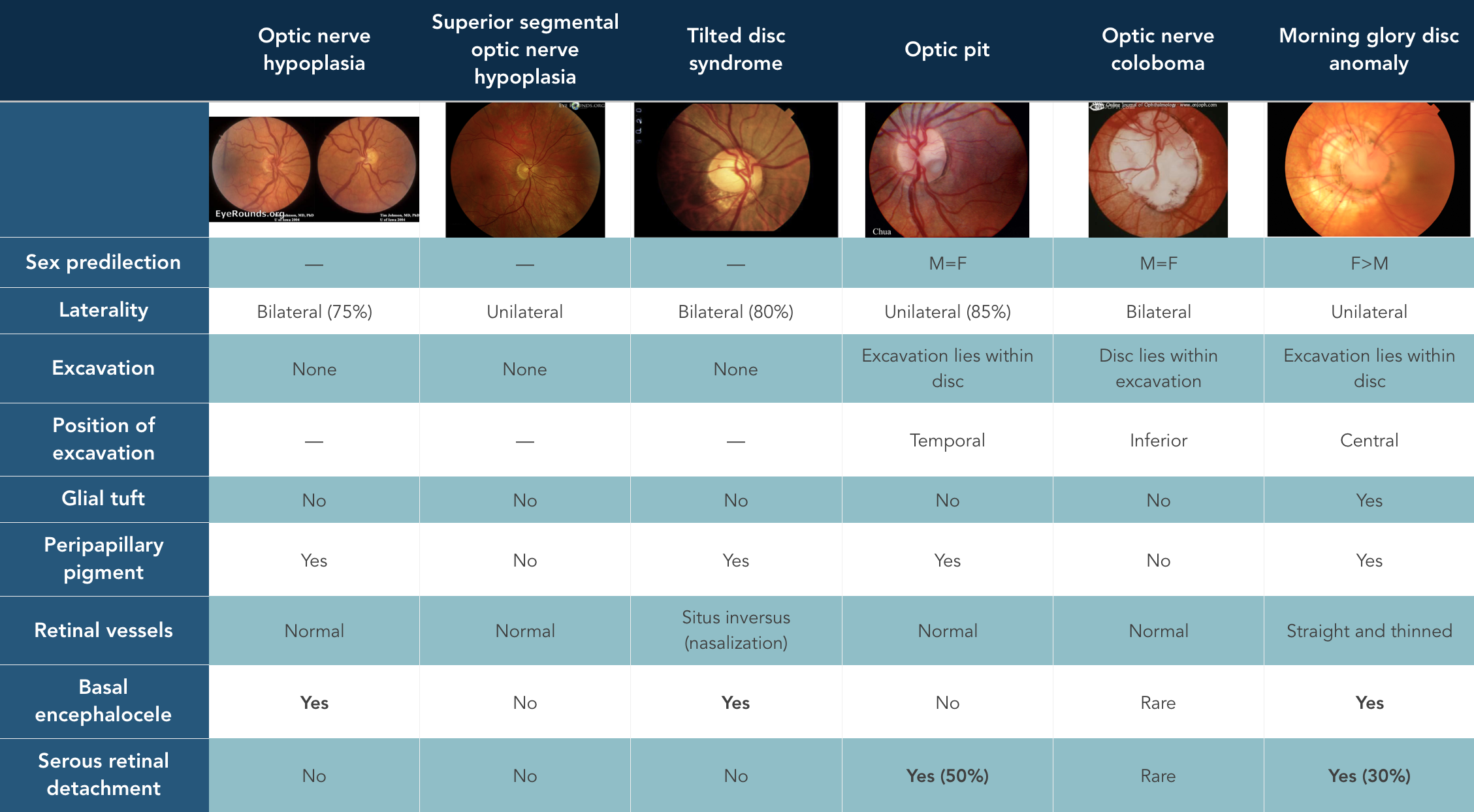
Summary
References and Additional Reading
- Basic and Clinical Science Course, Section 5: Neuro-Ophthalmology. American Academy of Ophthalmology, 2015.
- Al-Senawi R, Al-Jabri B, Al-Zuhaibi S, Al-Azri F, Al-Yarubi S, Harikrishna B, Al-Futaisi A, Ganesh A. Septo-optic dysplasia complex: Clinical and radiological manifestations in Omani children. Oman J Ophthalmol 2013;6:193-8
- Crotty TB, Campbell J, Sadun AA. Chapter 16: Pathology of the Optic Nerve. In: Duane's Ophthalmology on CD-ROM, 2006 Edition. Available online. Accessed 16 February 2016.
- Young RC, Tzu JH, Flynn Jr. HW. Optic pit maculopathy: Where is the fluid? Retinal Physician 2013;10:52,54-55.
Do you have any other hints to help remember congenital optic nerve anomalies? Did we leave anything out? Do you have suggestions or ideas for other topics? Leave a comment or contact us!