To help increase the amount of helpful study content on this site, I’ve partnered with some medical students from East Tennessee State University! They are being mentored by one of my former ophthalmology residents, Dr. Brent Aebi. The posts are primarily authored by the medical student, and reviewed/edited by myself and Dr. Aebi.
This post about HLA-B27 anterior uveitis was written by Suzanna Camp, B.S.
Overview
Human Leukocyte Antigens (HLA) are cell surface molecules that help the immune system distinguish between self and non-self.
HLA‑B27 acute anterior uveitis (AAU) is the most common form of non‑infectious anterior uveitis, representing 32% of AAU cases. It typically affects young adults (20s–40s) with male predominance (about 1.5–2.5x more compared to females). The risk of developing uveitis in the general population is 0.1%.
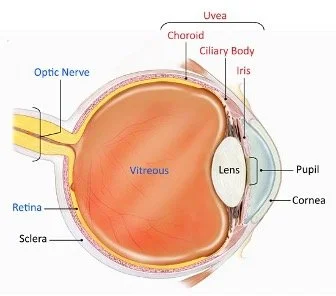
The uvea is composed of the iris, ciliary body, and choroid.
Image from the National Eye Institute.
HLA-B27-associated systemic conditions include:
Ankylosing spondylitis
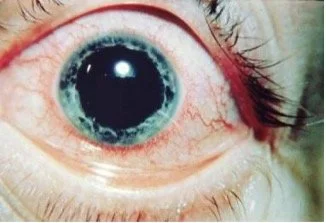
Acute anterior uveitis with ciliary flush in ankylosing spondylitis.
Image from Medscape.
Ranges from asymptomatic (only visible on x-ray) to severely symptomatic disease
Classic patient: young male with back and hip pain that improves with activity
90% of patients with AS are HLA-B27 positive
20-30% of patients will develop AAU
Reactive arthritis (Reiter’s Syndrome)
Patients present with “triad” of conjunctivitis, urethritis, and arthritis, with accompanying iritis in many cases (most patients do not have the triad)
The familiar med school mnemonic is “can’t see, can’t pee, can’t climb a tree”
Often occurs days to weeks after a GI or GU infection. Common bugs are Camplylobacter, chlamydia, Salmonella, and Shigella.
Other findings may include Achilles tendonitis, plantar fasciitis, and painless mouth ulcers. A characteristic skin finding is keratoderma blenorrhagicum (painful keratotic plaques on palms or soles of the feet).
30% of patients develop conjunctivitis.
3–12% of patients will develop iridocyclitis (inflammation of the iris and ciliary body)
This is a self-limited pathology (6-18 months) but recurs in 25-50% of patients, particularly in those who are positive for HLA-B27
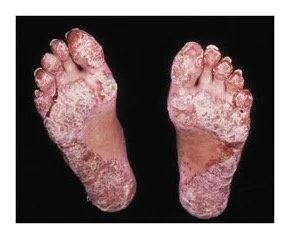
Keratoderma blenorrhagicum is a characteristic skin finding in reactive arthritis.
Image from The New England Journal of Medicine
Psoriatic arthritis
Psoriatic arthritis develops in 20% of patients with psoriasis.
Commonly presents as scaly, red rashes and pitted fingernails.
7-18% of patients develop uveitis
Unlike the other HLA-B27-associated conditions, psoriatic-associated uveitis is more likely to be bilateral, chronic, and can have posterior involvement.
Inflammatory bowel disease (IBD)
Ulcerative colitis (UC) and Crohn’s disease are the best-known syndromes that fall under the IBD umbrella. Both are characterized by recurrent and usually bloody diarrhea.
Both UC and Crohn’s can have ocular effects, but Crohn’s has been more frequently implicated than UC.
Episcleritis is the most common eye manifestation. This benign inflammation of the tissue covering the sclera can cause some pain and redness. It can spread to the sclera, causing scleritis.
Uveitis can develop slowly and bilaterally and can persist even in the absence of IBD flares
Some case studies have found that uveitis development could be associated with the use of anti-TNF drugs but no definitive connection has been made.
In the setting of bowel resection for IBD management, Vitamin A deficiency can develop, leading to night blindness.
Diffuse scleritis in a patient with IBD.
Image from World Journal of Gastroenterology
Clinical Presentation
Symptoms
Sudden onset of unilateral ocular pain, redness, photophobia, and sometimes blurred vision. Recurrence is common and has been documented to alternate between eyes.
Findings
Anterior chamber cell and flare
High magnification slit beam photo demonstrating cell and flare.
Image from Indian Journal of Ophthalmology.
Keratic precipitates
These are inflammatory cells that clump together and adhere to the inner surface of the cornea.
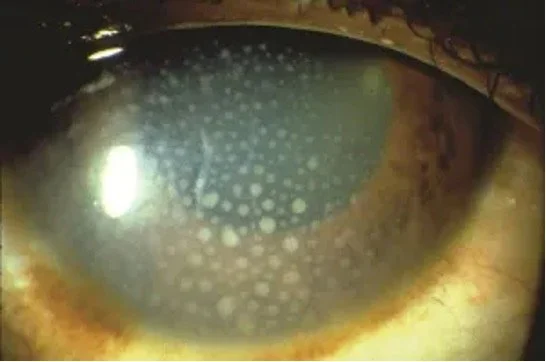
Keratic precipitates in anterior uveitis.
Image from American Academy of Ophthalmology.
Posterior synechiae
These are adhesions that develop between the iris and anterior capsule. These will occur in various inflammatory states, including uveitis.
Posterior synechiae in a patient with panuveitis.
Image from EyeRounds.
Hypotony during acute attacks
Hypotony develops from decreased aqueous humor production by the ciliary body due to inflammation. Increased uveoscleral outflow is another contributing factor.
In chronic uveitis, structural changes can occur, leading to membrane growth on the ciliary body.
Hypopyon and/or fibrin
Increased inflammation leads to a breakdown of the blood-aqueous barrier, resulting in protein leakage into the anterior chamber. In severe cases, an accumulation of inflammatory cells can aggregate within the anterior chamber (hypopyon). In later stages, fibrinous membranes can form within the anterior chamber.
Severe anterior uveitis with fibrinous reaction and hypopyon formation.
Image from Retina Image Bank.
Fibrinous membrane in the anterior chamber.
Image from Indian Journal of Ophthalmology.
Posterior Segment Involvement
Posterior segment involvement (vitritis, vitreous haze, choroiditis, or retinal vasculitis) occurs in up to 17% of HLA‑B27 cases.
Demonstration of vitreous haze.
Image from the International Journal of Retina and Vitreous.
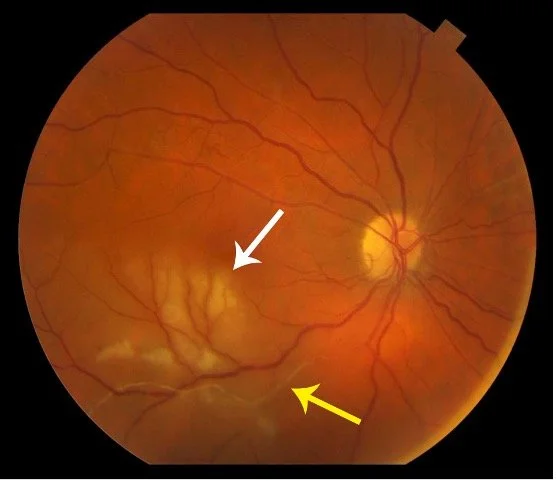
Fundus photo of choroiditis.
Image from Retina Associates.
Fundus photo of retinal vasculitis.
Image from University of Utah Moran CORE.
Diagnosis
The diagnosis of anterior uveitis is made by slit-lamp exam, confirming anterior chamber inflammation (cells, flare, precipitates)
Labs
When evaluating acute anterior uveitis, labs other than HLA-B27 are important for screening various etiologies:
Basic tests
CBC, CMP
Non-infectious tests
ESR, CRP, ANA, ANCA, ASCA
ACE and lysozyme
HLA-B27 screening
Infectious tests
Treponemal antibodies (with follow-up RPR/VDRL testing if positive)
QuantiFERON-Gold
Viral PCRs for EBV, HSV, CMV
Sacroiliac x-rays (as in ankylosing spondylitis)
“Bamboo spine” refers to squaring of the vertebrae
Chest x-ray and CT (important for sarcoidosis and TB consideration)
Rheumatology referral for co-management
Additional Tests
Depending on the patient history and in coordination with rheumatology, additional tests may be appropriate:
Ankylosing spondylitis: sacroiliac X-ray
“Bamboo spine” refers to the squaring of vertebrae
Sarcoidosis or tuberculosis (TB): chest X-ray, CT chest
Treatment and Management
Medical therapy
Corticosteroids
Topical corticosteroids (e.g. prednisolone acetate 1% or dexamethasone 0.1%)
May consider periocular steroids for cases of severe inflammation
Systemic steroids (oral or IV) may be considered with bilateral uveitis
Intravitreal steroids can be used in intermediate and posterior uveitis
Adverse effects: transient IOP elevation, cataract formation
Cycloplegic drops
Relieves pain from ciliary spasm
Prevents synechiae formation
Systemic immunomodulatory therapy
CellCept (mycophenolate)
Methotrexate
Anti-tumor necrosis factor (TNF) therapy has been shown to decrease recurrences of anterior uveitis
The first step in treatment is a topical steroid q1-6 hours in conjunction with a cycloplegic. If the response is inadequate, then we can consider periocular or oral steroids. The patient should be placed on a steroid tapering schedule based on the inflammation status.
Complications and Prognosis
Posterior synechiae formation
Best prevented with early cycloplegia and inflammation control
Cataract formation
Due to chronic inflammation and steroid use
Cystoid macular edema
Seen in 6% of HLA‑B27 uveitis cases
Uveitic glaucoma
Due to new synechiae formation, angle closure, and/or steroid use
Even with a high probability of recurrence, prognosis is usually favorable. Permanent vision loss occurs in only about 2.5% of patients who receive treatment.
References and Additional Reading
Chapter 5: Special Topics in Ocular Immunology In: Basic and Clinical Science Course, 2010-2011 Edition. American Academy of Ophthalmology.
Acute Anterior Uveitis - EyeWiki. eyewiki.org. https://eyewiki.org/Acute_Anterior_Uveitis
National Eye Institute. Uveitis | National Eye Institute. Nih.gov. Published 2019. https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/uveitis
Cliff Collins. NPF Advance Online. May 6, 2015. Uveitis: A Threat to Eyesight.
De Vicente Delmás A, Sanchez-Bilbao L, Calvo-Río V, Martínez-López D, Herrero-Morant A, Galíndez-Agirregoikoa E, Gonzalez-Mazon I, Barroso-García N, Palmou-Fontana N, Gonzalez-Gay MA, Hernández JL, Blanco R. Uveitis in psoriatic arthritis: study of 406 patients in a single university center and literature review. RMD Open. 2023 Jan;9(1):e002781. doi: 10.1136/rmdopen-2022-002781. PMID: 36635002; PMCID: PMC9843218.
Tiwari V, Brent LH. Psoriatic Arthritis. [Updated 2024 Jan 7]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK547710/
Troncoso LL, Biancardi AL, de Moraes HV Jr, Zaltman C. Ophthalmic manifestations in patients with inflammatory bowel disease: A review. World J Gastroenterol. 2017;23(32):5836-5848. doi:10.3748/wjg.v23.i32.5836
Haider D, Dhawahir-Scala FE, Strouthidis NG, Davies N. Acute panuveitis with hypopyon in Crohn’s disease secondary to medical therapy: a case report. J Med Case Rep. 2007;1:42. doi: 10.1186/1752-1947-1-42
HLA-B27-associated Acute Anterior Uveitis. EyeRounds.org: HLA-B27-associated Acute Anterior Uveitis. Uiowa.edu. Website. https://webeye.ophth.uiowa.edu/eyeforum/cases/334-HLA-B27-associated-Acute-Anterior-Uveitis.htm#gsc.tab=0
Ghassemi F, Nivousha MR, Hassanpoor N, Khoiasteh H. J Ophthalmic Vis Res. 2020 Jul 29;15(3):408–411. doi: 10.18502/jovr.v15i3.7459
CDC. Syphilis - STI treatment guidelines. www.cdc.gov. Published 2021. https://www.cdc.gov/std/treatment-guidelines/syphilis.htm
Chang JH, McCluskey PJ, Wakefield D. Acute anterior uveitis and HLA-B27. Surv Ophthalmol. 2005;50(4):364-388.
Cheeti A, Chakraborty RK, Ramphul K. Reactive Arthritis. [Updated 2023 Jan 2]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK499831/
Methotrexate Versus Mycophenolate Mofetil for Uveitis. American Academy of Ophthalmology. Published December 2, 2019. https://www.aao.org/eyenet/article/methotrexate-versus-mycophenolate-mofetil