To help increase the amount of helpful study content on this site, I’ve partnered with some medical students from East Tennessee State University! They are being mentored by one of my former ophthalmology residents, Dr. Brent Aebi. The posts are primarily authored by the medical student, and reviewed/edited by myself and Dr. Aebi.
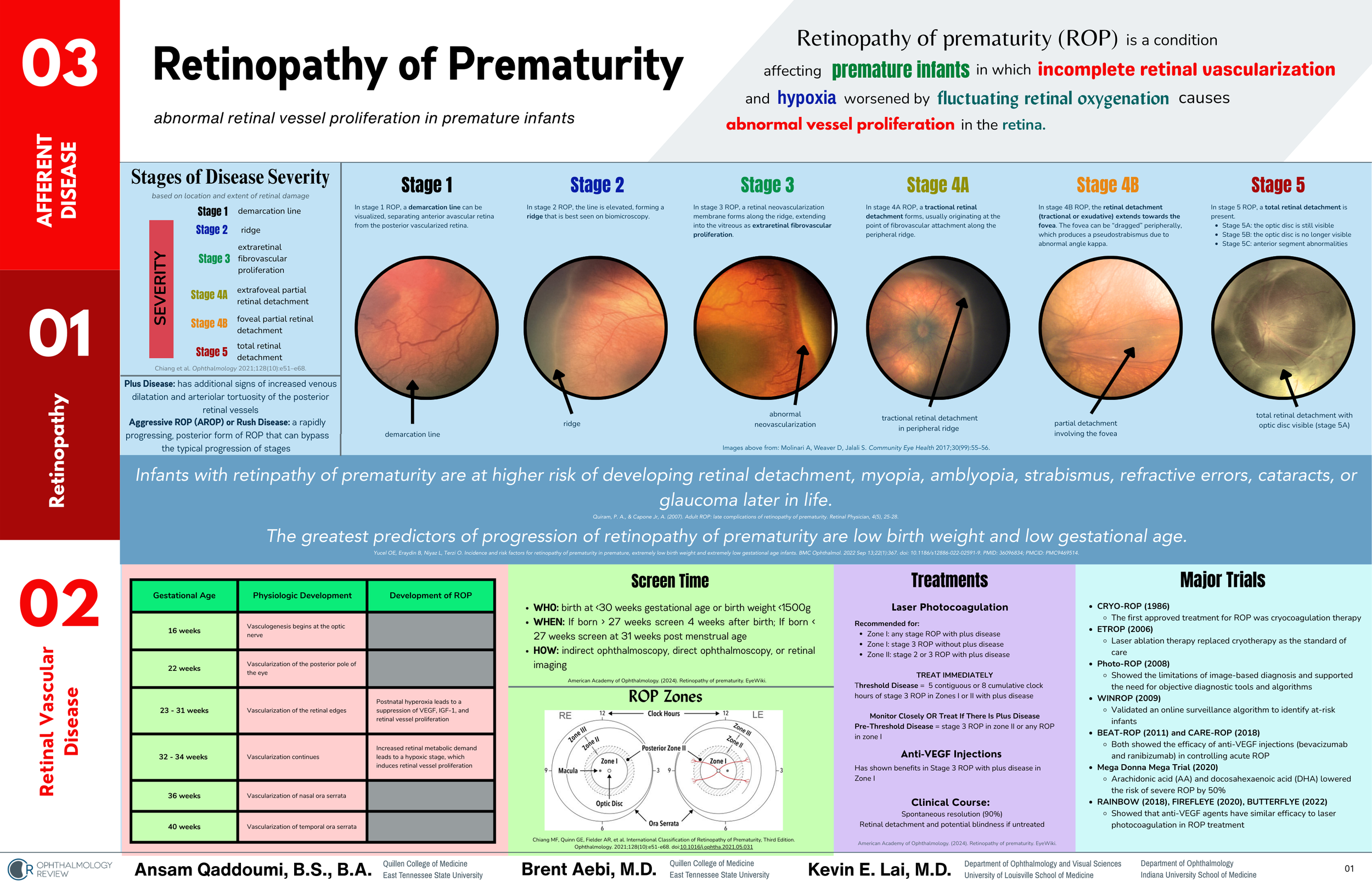
This post and one-page coffee table book excerpt about Retinopathy of Prematurity was written by Ansam Qaddoumi, B.S., B.A.